
Download the Case Study
See how a large academic Department of Medicine improved engagement, belonging, and team dynamics with KeepWOL.
 Case Study · Healthcare · Academic Medicine
Case Study · Healthcare · Academic Medicine
From Burnout Data to Belonging at Scale: A Department of Medicine Transformation
What started as a physician-led initiative to address documented belonging gaps grew into a year-long partnership now expanding across a large academic Department of Medicine spanning multiple clinical divisions, residency programs, and care teams across more than one campus.
Within the first quarter of department-wide rollout, engagement scores rose by more than 20% — one of six pillars showing measurable improvement
Leadership retreat participants saw job satisfaction rise by more than 35% after a single KeepWOL session — a leading indicator for retention
Engagement, team dynamics, job satisfaction, psychological safety, cultural intelligence, and innovation all improved within the first 90 days of rollout
A large academic Department of Medicine spanning multiple clinical divisions, residency programs, and care teams across more than one campus
Physicians, advanced practice providers, nurses, administrators, operations staff, and allied health staff across multiple campuses
One full year of structured deployment, beginning with quarterly leadership retreats, advancing to a department-wide rollout spanning multiple clinical divisions and care teams
Physician-led from day one. The department's Associate Chair of Belonging drove internal adoption and co-developed the implementation model
The Data Was Clear. The Path Forward Wasn't.
In 2023, the Department of Medicine analyzed its own All Staff Survey and identified a pattern that many large healthcare organizations recognize but few address with rigor: rapid growth, pandemic aftermath, and compounding burnout had eroded the conditions that make teams function well.
The lowest-scoring areas touched on the exact foundations of a healthy culture: whether leadership showed genuine interest in staff well-being, whether people felt free to speak their minds, whether they felt a strong sense of belonging, and whether they felt valued. To dig deeper, the department partnered with their enterprise Office of Belonging to conduct a comprehensive Organizational Network Analysis (ONA) of the physician workforce in 2024.
The ONA findings painted a clear picture of a department under strain, with persistent silos between divisions and campuses, generational disconnects across a multigenerational workforce, and meaningful pockets of staff who felt misaligned with the department's direction. Critically, the department had no existing mechanism to track progress in these areas or sustain any improvement over time.
Physician Burnout
Staff survey data revealed significant burnout among physicians, not as a future risk, but as a present reality affecting day-to-day performance and collaboration
Misalignment at Scale
A substantial portion of staff felt the department was not working toward a shared goal, undermining the cohesion needed to deliver exceptional patient care across a complex, multi-division structure
Persistent Silos
The ONA revealed structural disconnects between divisions and campuses, with key network connectors rated poorly at integrating newcomers and bridging teams
"These are not just data points. They're signals. Signals that something needs to change and that change must be intentional, measurable, and human-centered." — Department leadership
One Year. Three Phases. One Department Transformed.
This wasn't a single engagement. It was a deliberate, phased partnership that built evidence at each step before scaling. The department didn't just adopt KeepWOL. They designed a model of implementation that other departments could one day replicate.
Proving the Model at the Leadership Level
Before asking any team to participate, department leadership experienced KeepWOL firsthand, twice. Two executive wellness retreats brought together division chairs, nursing leaders, and operations administrators. Leaders saw measurable gains across all six performance domains, giving them the evidence and the confidence to move forward at scale.
A Department-Wide Pilot with Real Stakes
With leadership buy-in established and internal championship secured, the department launched a structured pilot across multiple teams and divisions. Baseline metrics were captured. Belonging Champions were identified within divisions. Facilitation models were tested, including KeepWOL-led, internally led, and hybrid approaches, to find the right balance of quality, cost, and scalability. A custom belonging survey, co-developed with internal teams, provided platform-independent validation of what was working.
Department-Wide Expansion Across 15 Divisions
Energized by pilot outcomes and armed with longitudinal data, the department moved toward a full-scale rollout spanning all clinical divisions and programs, reaching a large, multidisciplinary workforce across physicians, advanced practice providers, nurses, administrators, and allied health staff. Each division is supported by a trained Belonging Champion and a certified KeepWOL Facilitator. Real-time dashboards track performance at both the team and department level, enabling leadership to monitor trends, compare divisions, and make targeted adjustments throughout the year.
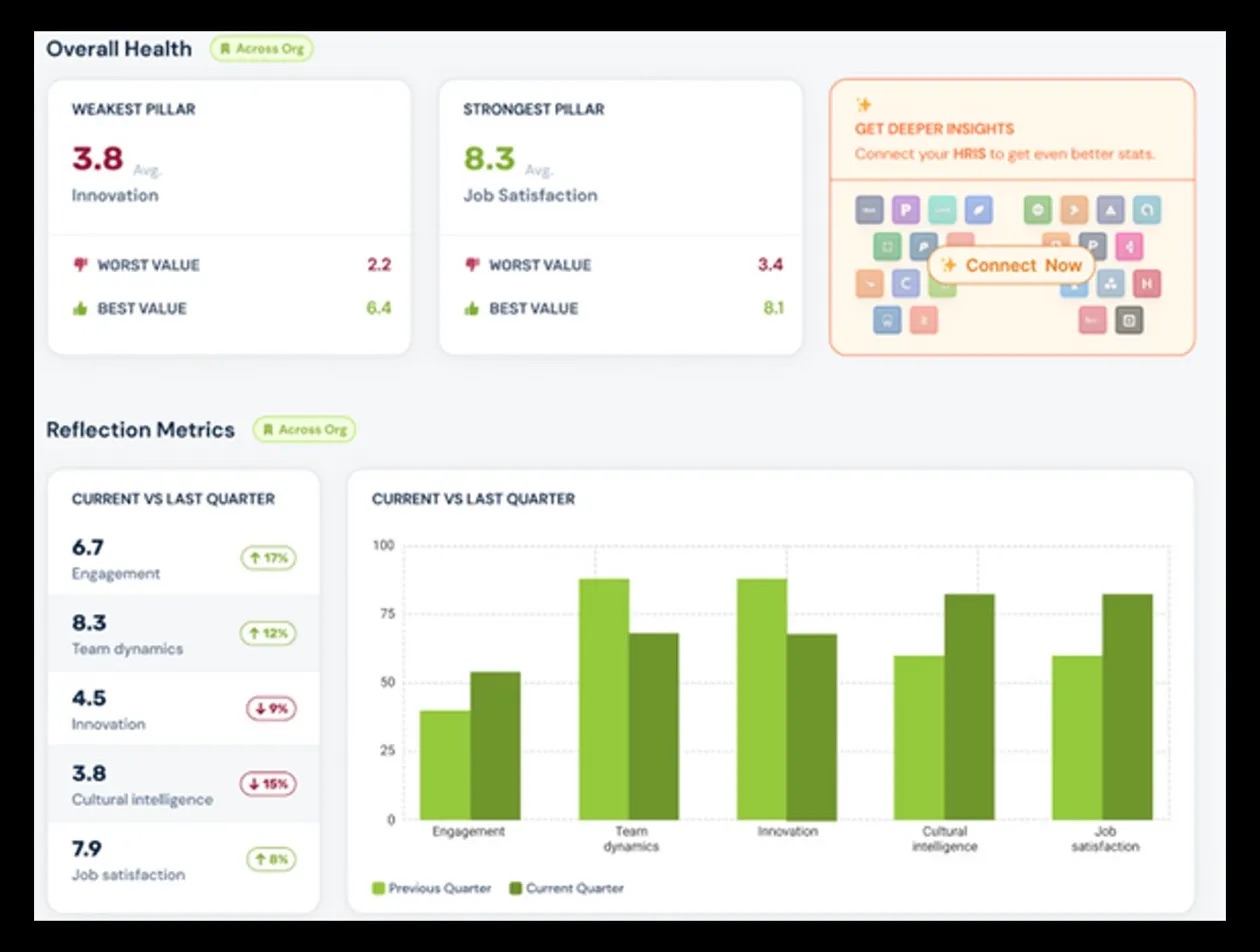
One Quarter In. Movement Across Every Pillar.
Just one quarter into the department-wide rollout, KeepWOL is delivering improvements across every performance pillar. Belonging, engagement, psychological safety, team dynamics, cultural intelligence, and innovation are all trending in the right direction. KeepWOL guarantees a minimum 10% improvement across all six pillars when the platform is used consistently for at least one year.
20%+ Engagement
Staff across divisions report feeling more connected to their teams and more motivated in their day-to-day work since KeepWOL sessions began
15%+ Job Satisfaction
Scores reflect a meaningful shift in how staff feel about their work environment, a leading indicator for retention in high-turnover healthcare settings
10%+ Team Dynamics
Cross-division collaboration and interpersonal trust are improving, addressing the silo patterns identified in the original ONA
5%+ Psychological Safety
Staff are speaking up more, sharing concerns earlier, and engaging more authentically, the conditions that underpin high-performing clinical teams
5%+ Cultural Intelligence
Awareness and appreciation of difference across a multigenerational, multidisciplinary workforce is measurably improving across participating teams
5%+ Innovation
Teams are generating more ideas and approaching problems more creatively, an early signal that psychological safety is taking root
KeepWOL guarantees a minimum 10% improvement across all six pillars when the platform is used consistently for at least one year. Results vary by team size, session cadence, and facilitation model. Contact us to discuss what outcomes are realistic for your organization specifically.
Before the Pilot Launched, Leaders Went First
Four quarterly executive wellness retreats gave division chairs, nursing leaders, and operations administrators a direct experience of what their teams would eventually participate in. Across a full year of leadership engagement, those who experienced KeepWOL firsthand became its strongest internal advocates. KeepWOL guarantees a minimum 10% improvement across all six pillars when used consistently, and leadership cohorts frequently see results well beyond that threshold.
35%+ Job Satisfaction
Marked improvement in how leaders felt about their work, even within a single session, signaling how quickly KeepWOL creates meaningful shifts
35%+ Team Dynamics
Division chairs and department leaders who rarely interact in a personal context began building real connections, breaking down leadership-level silos
20%+ Engagement
Leaders arrived at the retreat fatigued. They left re-energized, which is precisely the kind of shift that cascades down into how they show up for their teams
15%+ Cultural Intelligence
Even a single structured session surfaced perspectives and experiences that leadership hadn't shared with each other before, building genuine cross-cultural awareness
20%+ Psychological Safety
Leaders reported feeling more comfortable being honest with one another, an essential precondition for any culture change initiative to take root
20%+ Innovation
When people feel safe and connected, ideas flow. Leaders noted more generative conversation and creative problem-solving during and after their KeepWOL experience
Belonging is foundational to how physicians collaborate, support one another, and ultimately deliver the highest quality care to patients.
Associate Program Director, Internal Medicine Residency
Associate Chair of Belonging, Department of Medicine
Experience. Reflect. Grow. That's the Loop.
Every KeepWOL session follows a consistent three-stage framework that creates a repeatable, measurable cycle of team development. This is what makes KeepWOL sustainable rather than episodic. It isn't a retreat, a workshop, or a one-time training. It's an ongoing rhythm that builds over time.

Experience
Teams engage in AI-powered, facilitated interactive sessions designed to spark authentic conversation in a psychologically safe space. AI-generated prompts are tailored to the team's specific needs and context, whether that's onboarding, conflict, burnout, or cross-division collaboration.
Reflect
After each session, participants reflect individually and as a group. Quantitative scores across all six performance domains are captured in real time alongside qualitative goals, personal commitments, and group themes. This gives leaders a complete picture, not just what happened, but why it mattered.
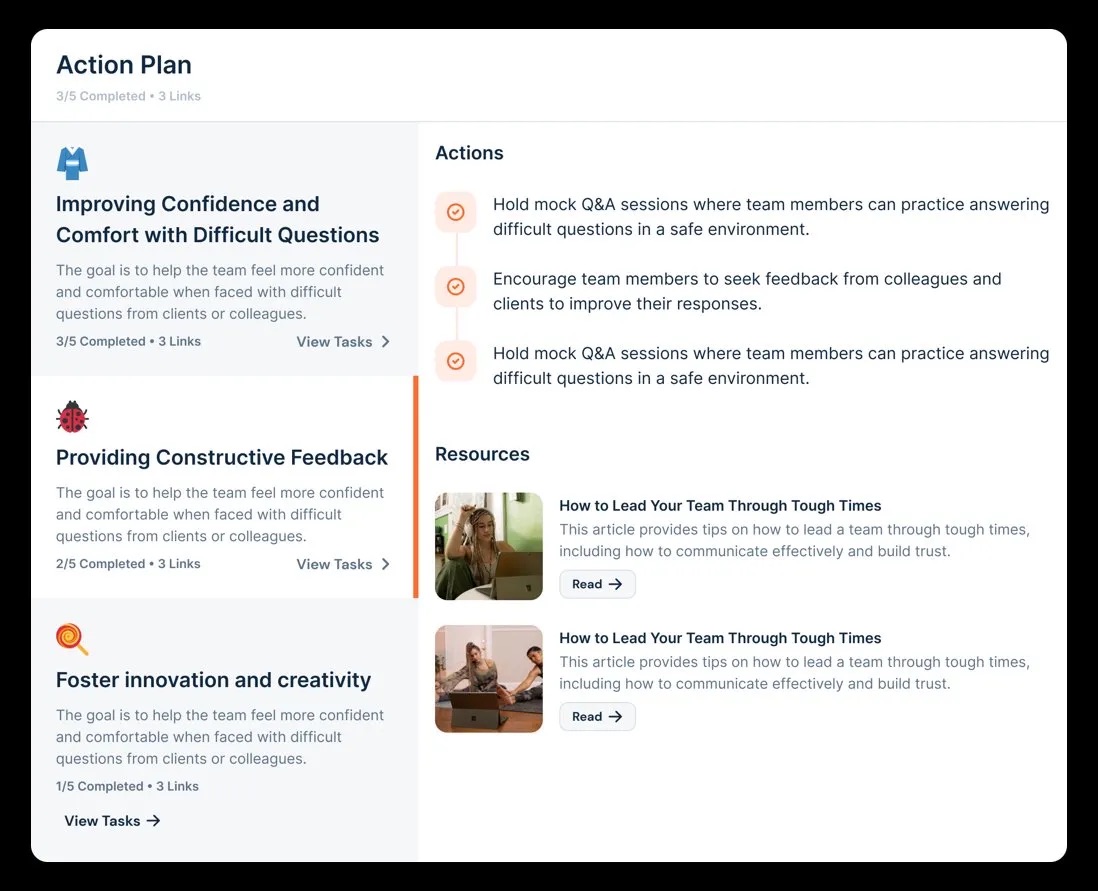
Grow
Data flows into longitudinal dashboards, enabling leaders to track monthly and quarterly trends, compare performance across divisions, identify bright spots or at-risk teams, and make targeted interventions. This is the visibility layer that most healthcare organizations have never had before.
One Department. One Shared Culture of Belonging.
The department's full expansion plan is built around sustainability, not just momentum. Three facilitation tracks give leadership the ability to identify the right approach for each team's size, culture, and available capacity. Session length is entirely at each team's discretion, ranging from 15 to 60 minutes. Some teams hold a dedicated monthly KeepWOL session, while others run a shorter session at the top of an existing multipurpose meeting to get everyone engaged and talking before turning to the agenda.
KeepWOL-Led
KeepWOL facilitates sessions directly. Ideal for divisions in the early stages of adoption where internal capacity isn't yet established.
Internally Led
Trained Belonging Champions within each division facilitate sessions independently, enabling full self-sufficiency and long-term scalability.
Hybrid
A blended model where KeepWOL provides oversight and coaching while internal facilitators lead the day-to-day experience.
The Belonging Champion Model
One of the most distinctive elements of this implementation is the Belonging Champion: a trained internal staff or faculty leader within each division who serves as the ongoing facilitator and culture steward for KeepWOL within their team. This isn't outsourced culture work. It's capacity built from within, with the tools, training, and data infrastructure to make it sustainable long after the pilot concludes. Each Champion is certified through KeepWOL's facilitator training program and receives ongoing support throughout the engagement.
This Is Physician-Led. Real-World. And It's Working at Scale.
What makes this engagement different from a typical team-building program isn't just the results. It's the model. This was not a top-down HR mandate. It was a physician champion who saw a problem in his own department, built the internal case with data, and partnered with KeepWOL to design something that would actually work in a complex clinical environment.
Built on Data, Not Guesswork
Every step of this engagement was grounded in the department's own survey data and ONA findings. KeepWOL didn't bring a generic solution. It met the department exactly where they were and built toward specific, measurable outcomes from day one.
Real-Time Cultural Visibility
Most healthcare departments have no ongoing mechanism to track belonging, psychological safety, or team dynamics. KeepWOL's dashboard gives leaders that visibility for the first time, monthly, quarterly, and at both the team and department level.
Scalable Across Any Division Size
From a small workgroup of six to a large division of hundreds, the platform flexes to meet teams where they are. Session length is at each team's discretion, from a focused 15-minute opener at the start of an existing meeting to a dedicated 60-minute monthly session. The three-track facilitation model ensures every team gets the right level of support without over-reliance on external resources.
Upstream Impact on Retention
Belonging, psychological safety, and engagement aren't soft metrics in healthcare. They're the upstream predictors of turnover, patient care quality, and institutional resilience. Improving them is an investment in the long-term performance of the organization.
Designed for Long-Term Sustainment
KeepWOL is not a one-time intervention. The Belonging Champion model, the internal facilitator network, and the ongoing dashboard infrastructure ensure the department can sustain and expand this work independently over time.
Structured Dialogue That Feels Human
Participants consistently report that KeepWOL surfaces conversations that wouldn't have happened otherwise. The structured interactive experience design is engineered to create psychological safety without feeling clinical or corporate.